
We are pleased to share our Litigation Matters publication, which highlights recent Canadian court decisions that may impact claims management in our industry.
This publication presents a comprehensive review of 22 reported Canadian judicial decisions involving Critical Illness (CI) insurance coverage issued between 2004 and 2025. It identifies judicial trends, evaluates the effectiveness of policy wording, and provides recommendations to reduce litigation risk.
General litigation data
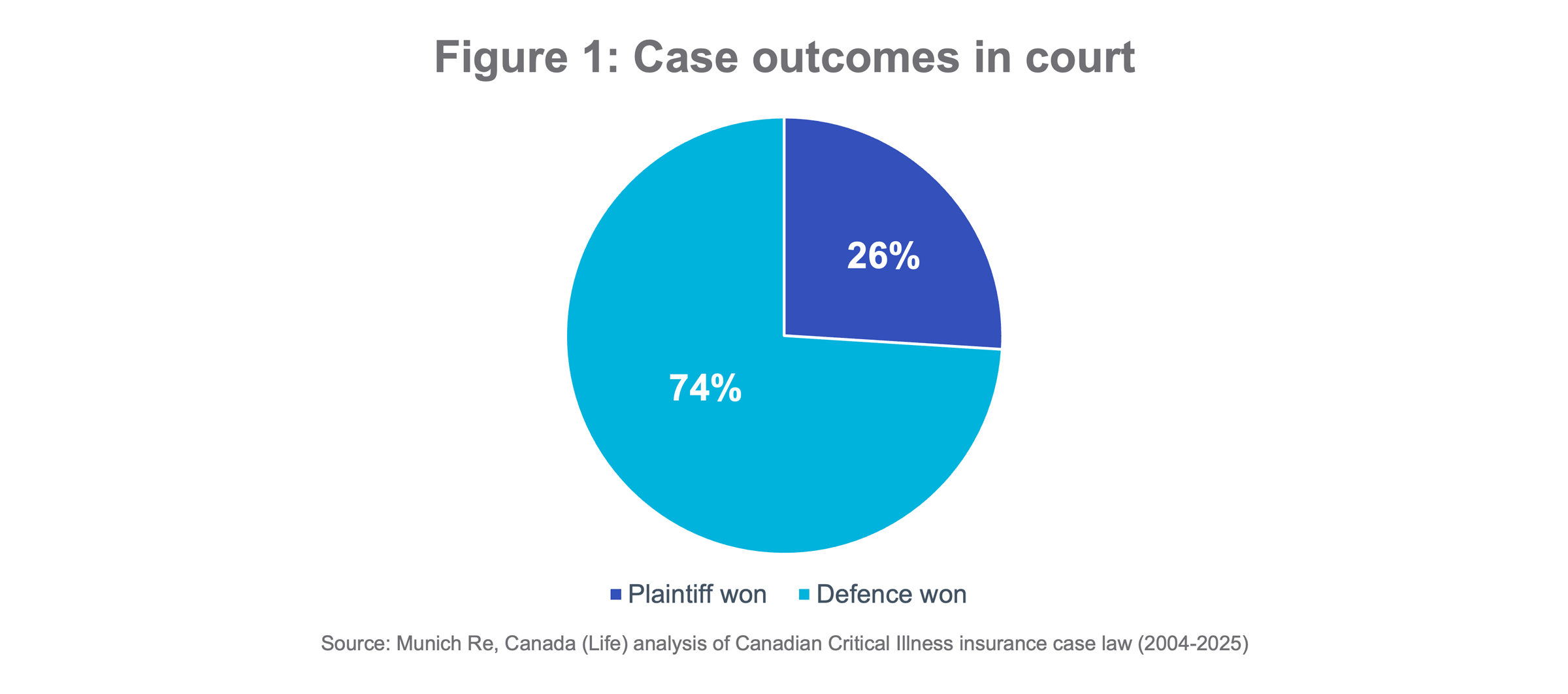
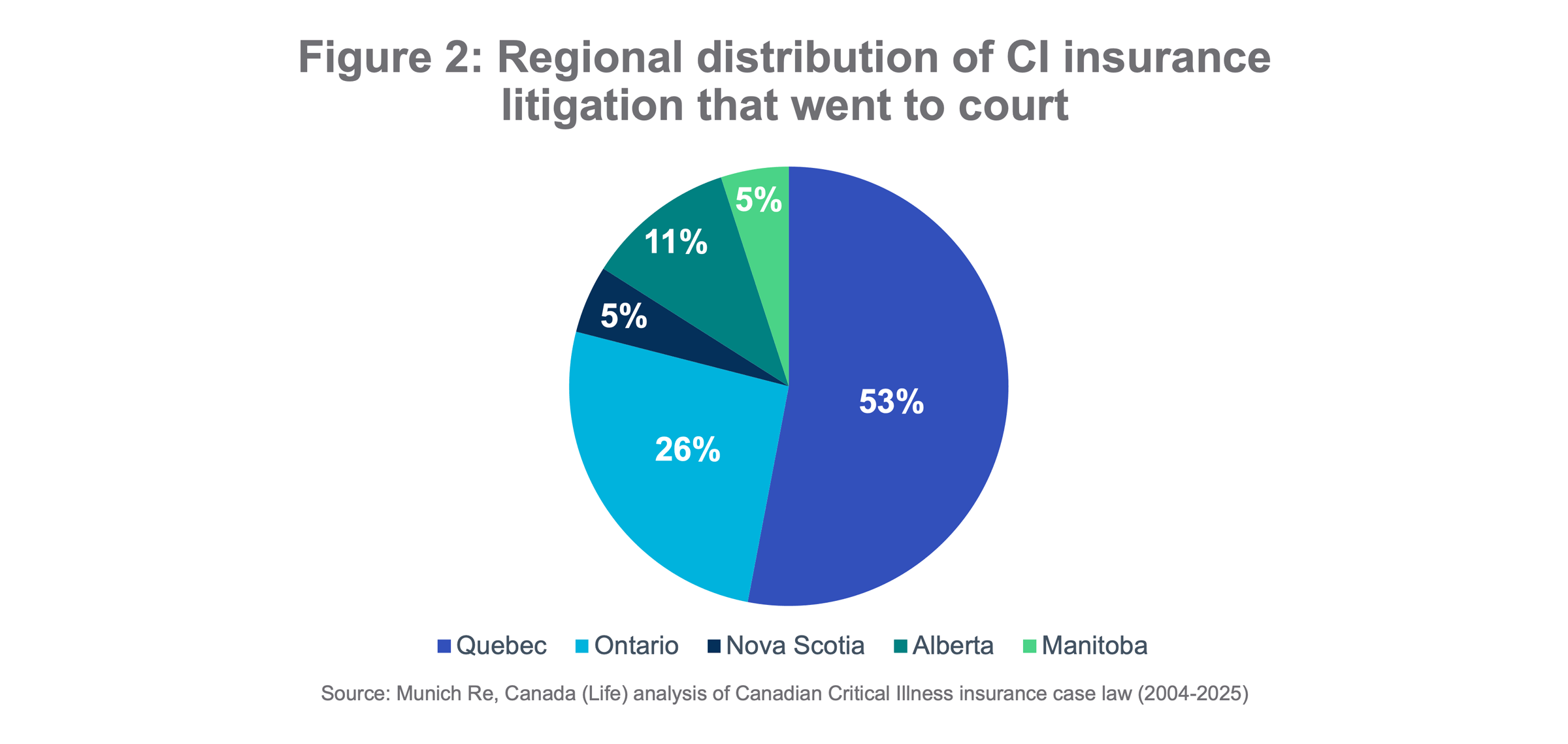
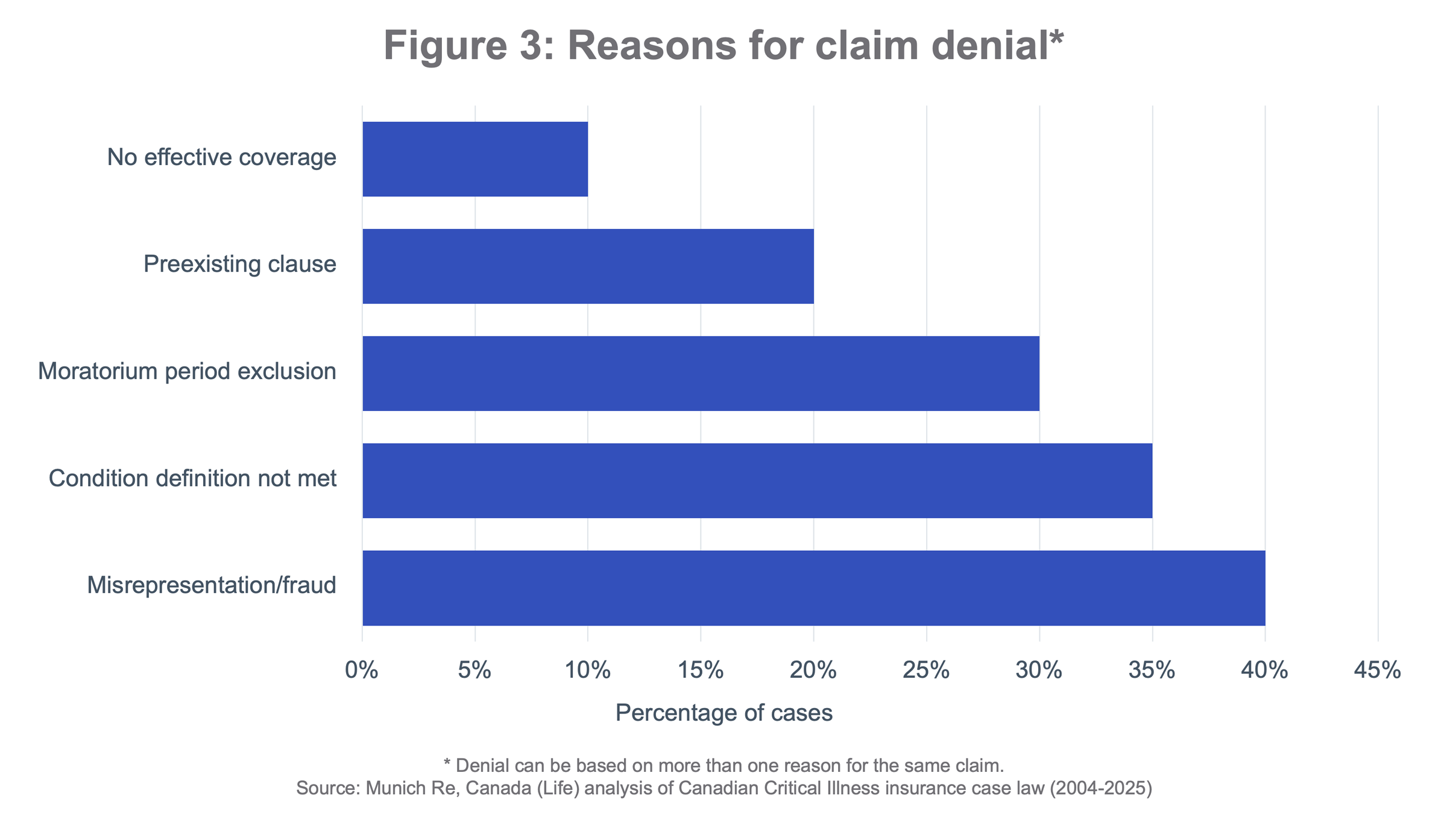
CI insurance case law analysis
Misrepresentation/fraud
Consistent with other lines of insurance business, courts have upheld the rescission of CI insurance policies for misrepresentation in the first two years following coverage inception (or its reinstatement with evidence), where applicants failed to disclose material information during the application process. The review of case law involving CI insurance coverage provides the following considerations, which may also be applicable for all lines of Life insurance business:
- An insurer can be entitled to rescind a policy based on medical misrepresentation when the undisclosed information would have led to a postponement of coverage (pending the stabilization of a medical condition or for completion of medical investigations) had it been disclosed at the time of underwriting.1
- To establish misrepresentation, courts have emphasized that health-related questions in the application must be clearly worded and easy to comprehend. In instances where ambiguity exists, judicial interpretation favors the claimant. In the case of MacQuarrie v. National Bank Life Insurance Company, 2014 ONSC 1298, which involved the rescission of a CI insurance policy, the health questionnaire required disclosure of any “respiratory disorder.” The plaintiff, who suffered from sleep apnea – - a condition material to the risk assessment – did not disclose it under that question. The Court accepted the plaintiff’s testimony that he understood sleep apnea to be a sleep disorder rather than a respiratory one. Accordingly, the Court found that the plaintiff answered the question truthfully based on his reasonable interpretation of the term “respiratory disorder.”2
- The burden of establishing policy rescission for misrepresentation applies equally to Simplified Issue products, a type of coverage increasingly offered in the industry for Life, Disability, and CI insurance. In Poulin v. Humania Assurances inc., 2017 QCCQ 4227 (CanLII), the Court held that rescission of the Simplified Insurance coverage is justified where it can be demonstrated that the coverage applied for would not have been issued had the relevant question been answered truthfully.
- A recently reported case involving CI insurance coverage arose from the Quebec Court of Appeal. It was the first CI insurance case in the Canadian industry that put the burden of proof on the insurer to establish fraud since the claim incurred beyond the two-year contestability period. In Paul-Hus v. Sun Life Canada, compagnie d'assurance-vie, 2025 QCCA 41 (CanLII), the Court of Appeal upheld the trial decision, finding that the insured had failed to disclose material medical history at the time of application, despite clear and specific questions. Sun Life successfully demonstrated that the insured knowingly misled the insurer to obtain coverage, thereby distorting its risk assessment.3
Preexisting condition clause in CI insurance
The pre-existing condition clause is typically found in Group CI insurance coverage issued without health evidence and may also appear in individual Simplified Issue CI insurance policies. Under CI insurance coverage, this clause usually applies to claims made within the first 24 months from the start of coverage and requires a review of the medical history covering the 24 months preceding the coverage inception.
Since it is an exclusion clause, the pre-existing condition provision is subject to restrictive judicial interpretation, typically favoring the insured. Accordingly, it is imperative that the clause be drafted with sufficient clarity and breadth to exclude coverage where, during the pre-existing period, there is evidence of symptoms, signs, treatments, medications, or investigations related to the claimed condition, even in the absence of a formal diagnosis.
Case law involving CI insurance claims denied under the pre-existing condition clause reveals a significant burden of proof on the insurer. To succeed in court, the insurer must establish, on a balance of probabilities, that the claimed condition existed in the period covered by the preexisting clause and could not reasonably be attributed to another condition. Courts have held that if medical records indicate it was too early to confirm the condition or suggest alternative diagnoses, this may be sufficient to preclude the application of the clause.4
90-day Moratorium Period (MP) exclusion for cancer
The 90-day MP exclusion clause applicable to cancer claims is part of the Canadian Life and Health Insurance Association (CLHIA) Benchmark definitions and has been in use across the industry since 2008. It provides that if symptoms, signs, or medical investigations leading to a diagnosis of cancer occur within 90 days following the effective coverage date, the claim can be denied even if the diagnosis is made after the 90-day period.5
Courts have repeatedly upheld the validity of the Benchmark 90-day MP exclusion clause, confirming that its wording is not ambiguous, does not create a discrepancy between the application of coverage and the policy, and serves to prevent anti-selection.6
In Talbot v. Industrielle Alliance, assurance et services financiers, 2020 QCCS 193 (CanLII), the court reminded that if the application of the 90-day MP exclusion clause also includes a permanent exclusion for any future cancer, such exclusion needs to be clearly worded in the 90-day MP exclusion clause and in the provision including all policy exclusions.
Condition not meeting definition
The review of the case laws involving CI claims denied because the plaintiff’s condition did not meet the applicable policy definition shows that heart attack definitions are among the most frequently challenged in Canadian courts.7
Menard v. The Canada Life Assurance Company, February 19, 2004, Ont. S.C.J. was the first Canadian case law involving CI insurance coverage. The insurer denied the claim since it was not covered by the policy definition for heart attack, which required as the main criteria new changes in the electrocardiographic (ECG) indicative of a myocardial infarction.
The Court underscored the concern that ECG changes may not always be present in individuals who suffered a myocardial infarction. It accepted the plaintiff’s argument that medical progress has shown that one cannot rely solely on ECG changes as a diagnostic criterion, as this would exclude all non-ST-elevation myocardial infarctions. The Court ruled in favour of the plaintiff, affirming that the principal diagnostic criterion should be the rise and fall of biochemical cardiac markers, specifically troponin levels, consistent with myocardial infarction.
In 2008, the inaugural version of the CLHIA Benchmark Definition for Heart Attack reflected advancements in medical diagnostics by recognizing the rise and fall of biochemical cardiac markers to thresholds consistent with myocardial infarction as the primary criterion for establishing a diagnosis along with at least another medical criterion.8
Canadian courts have had the opportunity to assess the validity of the CLHIA Benchmark Definition for Heart Attack. In most cases, they concluded that the definition was not met based on the specific medical evidence presented. Notably, in Afzal v. National Bank of Canada, 2014 ONCA 26 (CanLII), the Ontario Court of Appeal affirmed that the absence of a concurrent elevation in troponin levels alongside ECG changes was indicative of a prior myocardial infarction and did not satisfy the policy’s definition of a covered heart attack event.
Judicial takeaways for underwriting and claims operations
Policy drafting
- Health questions must be drafted using clear, unambiguous, and easily understandable language. Any ambiguity in the wording may be interpreted in favor of the plaintiff in court proceedings.
- The pre-existing condition clause must be tightly and precisely drafted to ensure it applies even in cases where no formal diagnosis was made during the preexisting period. The clause should clearly encompass symptoms, medical consultations, treatments, or any indications of a condition – regardless of whether a diagnosis was established – to avoid interpretive gaps that could be challenged in court.
- Incorporate the Benchmark 90-day Moratorium Period exclusion in the definition of the covered condition and in the contract section including all applicable exclusions. If applicable, also include clear wording excluding any future claim for cancer (or benign brain tumor).
Claims handling
- When denying a claim, consider all applicable grounds for denial. Ensure that each ground is clearly stated in the denial letter sent to the claimant.
- Courts consistently uphold the application of the Benchmark 90-day Moratorium Period exclusion. Therefore, when this exclusion is applicable, it is essential to reference it explicitly in the rationale for claim denial.
Do you have comments on this publication? Would you like us to write an article on a particular subject, or are there any legal issues you would like us to discuss in a future publication? Please tell us what interests you and share your comments by writing to us.
This article is for informational purposes only. It should not be relied upon and is not intended to constitute legal advice.
References
1See Hamideh v. Industrielle Alliance, assurances et services financiers inc., 2016 QCCS 631 (CanLII); Axa Assurances inc. v. L.S., 2013 QCCA 490 (CanLII).
2The claim was however denied due to the application of the 90 days Moratorium Period exclusion, which was confirmed by the Court of Appeal in MacQuarrie v. National Bank Life Insurance Company, 2015 ONCA 100 (CanLII).
3The trial decision in Paul-Hus v. Sun Life Canada, compagnie d'assurance-vie, 2023 QCCS 3890 (CanLII), was summarized and discussed in our previous publication Litigation Matters, dated December 2024.
4See Brouard v. Sun Life du Canada, compagnie d'assurance-vie, 2014 QCCQ 1358 (CanLII); MacQuarrie v. National Bank Life Insurance Company, 2014 ONSC 1298 (CanLII).
5The 2024 version of the CLHIA Benchmark definitions also includes Moratorium Period exclusion clauses for benign brain tumor - 90 days, MS -one year, and Parkinson’s Disease - one year.
6See Masson v. Desjardins Sécurité Financière, Compagnie d'assurance vie, 2023 QCCQ 3699 (CanLII), Talbot v. Industrielle Alliance, assurance et services financiers, 2020 QCCS 193 (CanLII), Camiré v. Desjardins Sécurité financière, 2018 QCCS 1503; confirmed in Appeal in Camiré v. Desjardins Sécurité financière, 2020 QCCA 749 (CanLII), Provenzano v. Great-West Life, 2013 ONSC 5254, Assurance-vie Banque Nationale v. Tremblay, 2011 QCCA 629 (CanLII).
7See Fusinato v. Compagnie d'assurances du Canada sur la vie, 2016 QCCS 1187 (CanLII); Afzal v. National Bank of Canada, 2014 ONCA 26 (CanLII) confirming Afzal v. National Bank of Canada, July 14, 2012, Ont. S.C.J.; Sauvage v. Desjardins Assurances (Desjardins Sécurité financière, compagnie d’assurance vie), 2016 QCCQ 17272 (CanLII); Funk v. Blue Cross Life, 2015 MBQB 184 (CanLII); Menard v. The Canada Life Assurance Company, February 19, 2004, Ont. S.C.J.
8Severe Heart Attack* (acute myocardial infarction) is defined as a definite diagnosis of death of heart muscle due to obstruction of blood flow, that results in:
Heart attack symptoms, accompanied by a rise and fall of cardiac biomarkers to levels considered diagnostic of acute myocardial infarction, with at least one of the following:
- New electrocardiographic (ECG) changes consistent with an acute myocardial infarction;
- New diagnostic imaging changes consistent with an acute myocardial infarction;
- Development of new pathological Q waves on ECG after an intra-arterial cardiac procedure including, but not limited to, coronary angiography and/or angioplasty.
Exclusions specific to Severe Heart Attack: No benefit will be payable under this condition if:
- ECG changes are suggestive of a prior myocardial infarction;
- Other acute coronary syndromes, including angina pectoris and unstable angina are diagnosed;
- Elevated cardiac biomarkers and/or symptoms result from medical procedures or diagnoses other than acute myocardial infarction.
The diagnosis of severe heart attack (acute myocardial infarction) must be made by a Specialist.
Contact the author

This may interest you
properties.trackTitle
properties.trackSubtitle



