properties.trackTitle
properties.trackSubtitle
The health insurance world is complex and evolving
Today’s health insurance companies face a highly competitive and complex landscape. Technology is changing rapidly. Regulatory requirements are complicated and evolving. And customers are demanding more and better products and services. It can be hard to keep up.
To stay competitive and relevant in the industry, health insurers must innovate, manage risk, and engage with new customers constantly. But they can’t do that if they depend on legacy systems and processes. They need a business transformation with technology investments that unlock potential and enable growth.
Who you choose as a partner is key to your transformation’s success.
More than 100 insurance companies around the globe undertake system replacements or transformational projects each year. Many fail or are significantly delayed due to several reasons including the selection of the wrong partner or product.
To successfully transform your systems, you need a product and a vendor who will fit your business culture and requirements.
MEDNEXT is the solution you need
MEDNEXT is an innovative end-to-end, sophisticated, robust and functionality rich Health Insurance Management System for health insurance players. It empowers health insurers to tackle the challenges of today and tomorrow by providing a robust and intuitive user interface, advanced automation, increased integration, customization and configuration capabilities and extended support for both global and local provider networks. For more than 25 years, insurers have trusted MEDNEXT to help them create new products and services and bring them to market quickly.
MEDNEXT supports:
- Any individual or group health insurance product, including group life and critical illness benefits
- Insurers of all sizes for domestic and iPMI (International Provider Medical Insurance) lines of business
MEDNEXT is the Health Insurance Management System you need to manage your entire book of business. It is cloud-ready, supports multiple currencies and is scalable to grow as you do, giving you the agility to adapt and excel in today’s ever-changing insurance marketplace.
Munich Re HealthTech Named a Luminary in the 2022 Global Celent Health Policy Administration Systems report and won the XCelent Customer Base and Support Award
How you benefit from MEDNEXT.
Taking the complexity out of the health insurance business
Give your management, operations and IT teams peace of mind with MEDNEXT. This complete, off-the-shelf software solution can automate health insurer’s business processes from start to finish, from product configuration to sales and distribution, to policy administration and claims management.
In fact, with MEDNEXT, you can:
- Empower your users to configure even the most complex health products, without IT help
- Manage the entire policy administration process, from quotation to renewal, improving operational efficiency and customer experience
- Automate your authorization and claims management process, increase straight-through process, improve turnaround time and reduce claim costs
- Handle multiple provider networks with different contracts, SLAs and pricelists
- Integrate seamlessly with a Business Intelligence (BI) system, enhancing the platform's' capabilities to monitor operations, provide transparency to business executives, and empower self-service creation of analytics and reporting.
- Leverage your existing investments with MEDNEXT API extended connectivity and integration capabilities
Key features & capabilities to manage your business
Product Configuration Module
No need for programming or specialized IT support to configure any health insurance product.
Quotation & Application Module
Option-driven quotation and easy management
of policy info, member demographic, and medical data for solid underwriting decisions integrated automatically into the premium and the claim process.
Enrollment Module
Dynamic customer, policy and member structures with a robust premium engine, to help you manage any policy from start to finish.
Claims Adjudication Module
Powerful claim adjudication engine allowing you to fully automate the claims process, increase customer satisfaction and reduce claims costs.
Medical Provider Module
Simple management of different providers and contracts, handling of multiple networks with different rates. Improved customer and partner experience through automation.
Authorization Module
Easy administration of medical cases and management of information about member in-patient and outpatient treatments and pre-approvals.
Sales & Commissioning Module
Easy management of distribution channels, automatic and effective calculation of commissions.
Billing Module
Flexible billing module to enable you streamline the billing process, create detailed invoices, and accurately optimize collections.
Reinsurance Capabilities Module
Application of reinsurance in any product or product component including packages, plans or benefits.
Technology for today and the future
Health insurance companies count on MEDNEXT to provide a modern, service-centered software system to support their digital ecosystems.
Today, MEDNEXT leverages Oracle’s technology stack to ensure peace of mind far into the future. MEDNEXT provides extensive set of APIs and to extend our customers’ integration capacities, enabling them to create and operate a health insurance ecosystem. We’re excited to include additional cutting-edge features in our roadmap, as well as new capabilities proposed by our Munich Re Health Tech Community members, through an annual product ideation process.
Deployment and licensing options that work best for your business
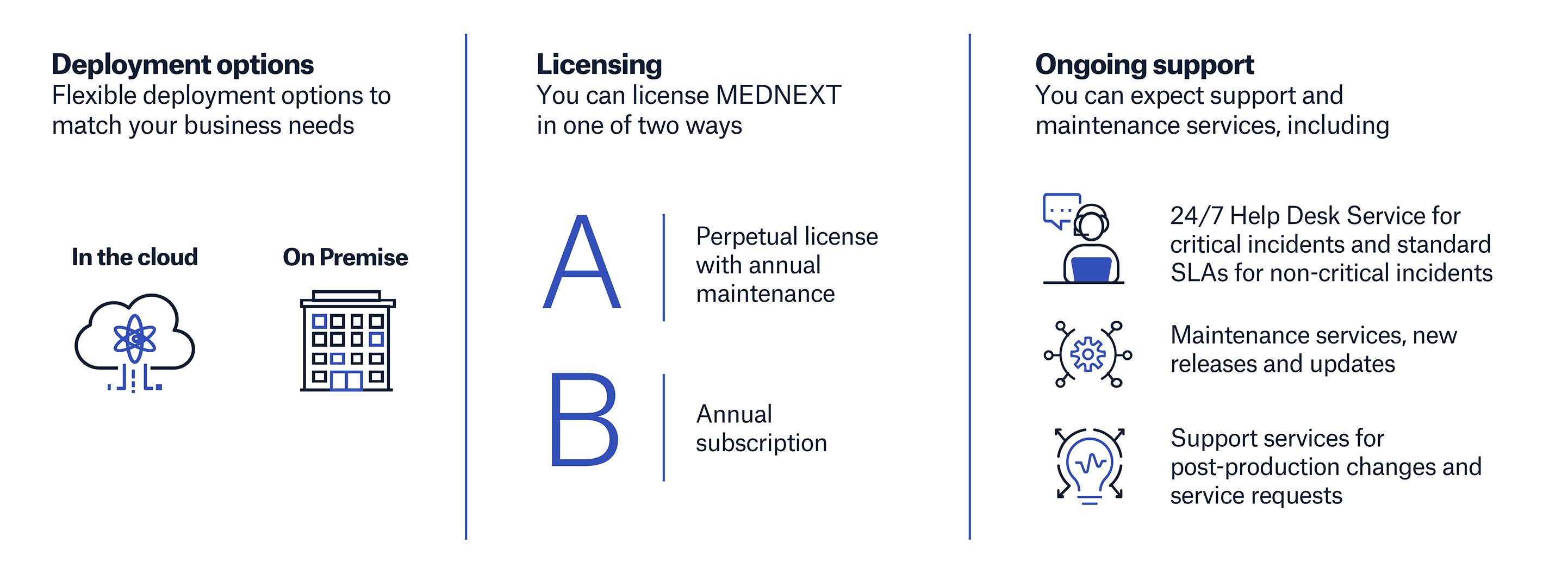
The path to your business transformation
Below are the steps we will take as part of our methodology
- Discovery call or meeting – We identify your business need and ensure that MEDNEXT is a good match.
- Pre-sales engagement – We work to deeply understand your need and demonstrate how we can address it, through custom demos, presentations or product documentation.
- Agreement – We put our agreement in writing, ensuring there is transparency and tight governance in every step of our future relationship.
- Implementation – We deliver on our promise on time and within budget.
- Support – Our Help Desk ensures that you have answers to your questions, according to the SLAs.
- Account management – We assign you an account manager. He or she will act as your single point of contact, ensuring we always meet our obligations and keep you happy.
MEDNEXT at a glance
19 entities around the globe
in Europe, Middle East, Latin America and Africa
2,500 users
worldwide
5.5 million
members supported
30 million claims
processed per year
€1.5 billion
Premiums collected
.jpg/_jcr_content/renditions/original./iStock-1280956095%20(Static).jpg)
