
Background
Electronic Health Records (EHRs) represent a significant data innovation in modern life underwriting, but achieving their full value depends on how they are used. As carriers invest in accelerated and fluidless programs, understanding which evidence sources deliver the strongest balance of speed, cost, and risk protection has become increasingly important; particularly as time to issue and underwriting expense remain key competitive considerations.
Traditional underwriting processes, even in accelerated and modified programs, may rely on a standard set of requirements based on approved age and amount grids. While additional underwriting evidence may improve risk assessment, each requirement carries incremental time and cost implications. In some cases, adding evidence such as an attending physician statement (APS) may mitigate mortality slippage but undermine the core objectives of accelerated underwriting by increasing friction, costs, and time to issue. As a result, it is critical to evaluate which evidence sources balance protective value against successful program design.
Building on prior Munich Re retrospective research assessing the protective and operational benefits of EHRs, we sought to address a more fundamental question: could introducing EHRs early in the accelerated underwriting process allow carriers to expand eligibility, increase straight‑through processing, and reduce mortality slippage — while also improving cost and cycle time efficiency? More specifically, can carriers capitalize on the depth and breadth of information contained within EHRs, including prescription and medical claims data, clinical lab results, and, in some cases, test results and office notes, while staying within the speed-to-decision goals associated with accelerated underwriting (AUW) cases?
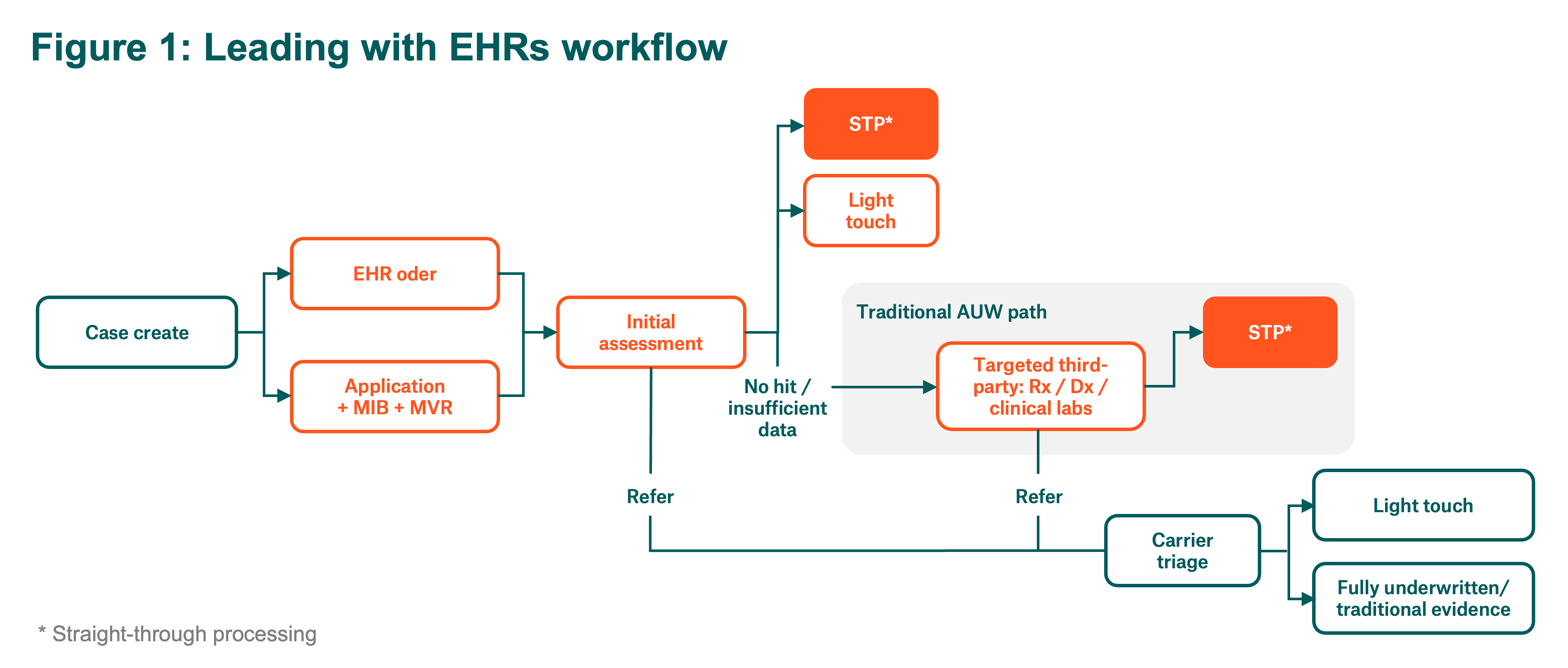
This analysis evaluates the protective and operational value of Leading with EHRs, defined here as adding EHRs as one of the first piece of underwriting evidence within the workflow (in place of prescription and medical data), as well as reflexively ordering the missing information when EHRs lack the evidence needed to render an underwriting decision (Figure 1).
Key findings
- Within a study population limited to applications with a valid EHR, positioning EHRs as the first piece of evidence in underwriting, supported by reflexive ordering of additional information when needed, enables underwriting decisions to be made for 20% more policies compared with a traditional AUW program where an EHR is not used as underwriting evidence.1
- Further analysis shows that using an EHR as the first piece of underwriting evidence results in a 25% improvement in mortality outcomes relative to a traditional AUW program.
- Altogether, Leading with EHRs has the potential to deliver $781 in total savings per application across mortality, evidence, and underwriting time. Mortality protection is the primary driver of these savings. Additional benefits are outlined in Table 1.

Data and methodology
This paper evaluates the benefits of positioning EHR data as the first piece of evidence ordered on an applicant in the underwriting process, in combination with application disclosures (applicant’s admitted history), MIB activity, and motor vehicle record (MVR) checks within the accelerated underwriting workflow. Munich Re defines accelerated underwriting as lab-free underwriting, which utilizes an applicant’s disclosure in conjunction with data vendor tools to render a faster underwriting decision. The use of APS can often lengthen the underwriting process from a few days to a few months. For the purpose of the study and our subsequent findings, APS would not leverage the same cost and time savings as EHRs.
Our study was based on a random sample of 144 of the 800 life insurance applications from multiple carriers used in earlier retrospective studies.2 Underwriting files consisting of business from multiple carriers targeting middle to high-net-worth markets. Broker, general agency, and direct-to-consumer distribution channels were included, as were traditional and fluidless underwriting paths. For this analysis, we required cases that returned electronic health data.
The study captures the underwriting risk class assessment for two simulated underwriting programs, Traditional AUW and Leading with EHRs, as outlined in Figures 2 and 3.
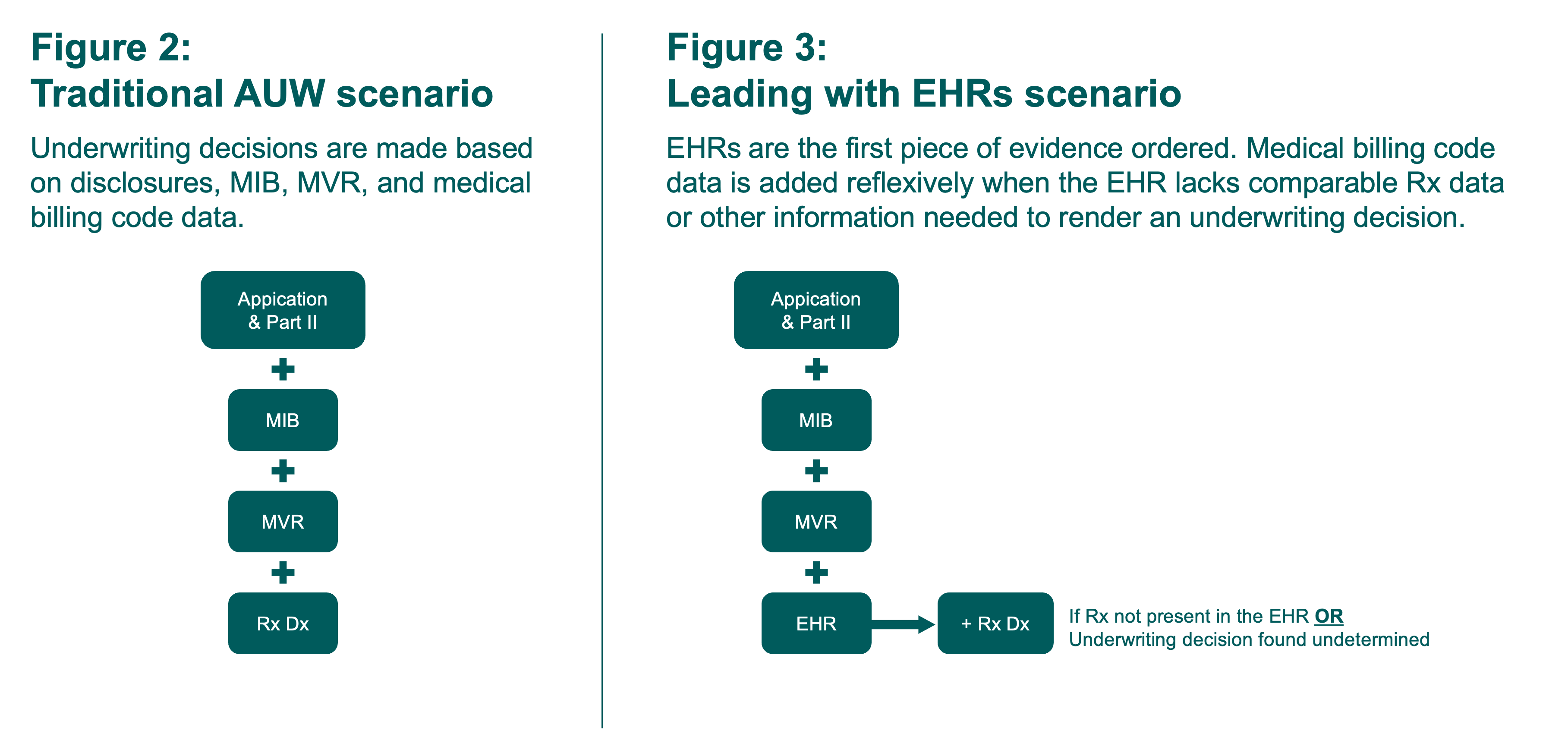
To ensure an independent review, we engaged both external and internal underwriting consultants to assist with completing the risk assessments. For consistency, they used the Munich Re MIRA Pro underwriting manual to assess risk in each scenario.
Munich Re calculated the expected mortality based on the underwriting risk class decisions for both simulated programs. The following methodology was used to quantify mortality savings and perform a cost-benefit analysis.
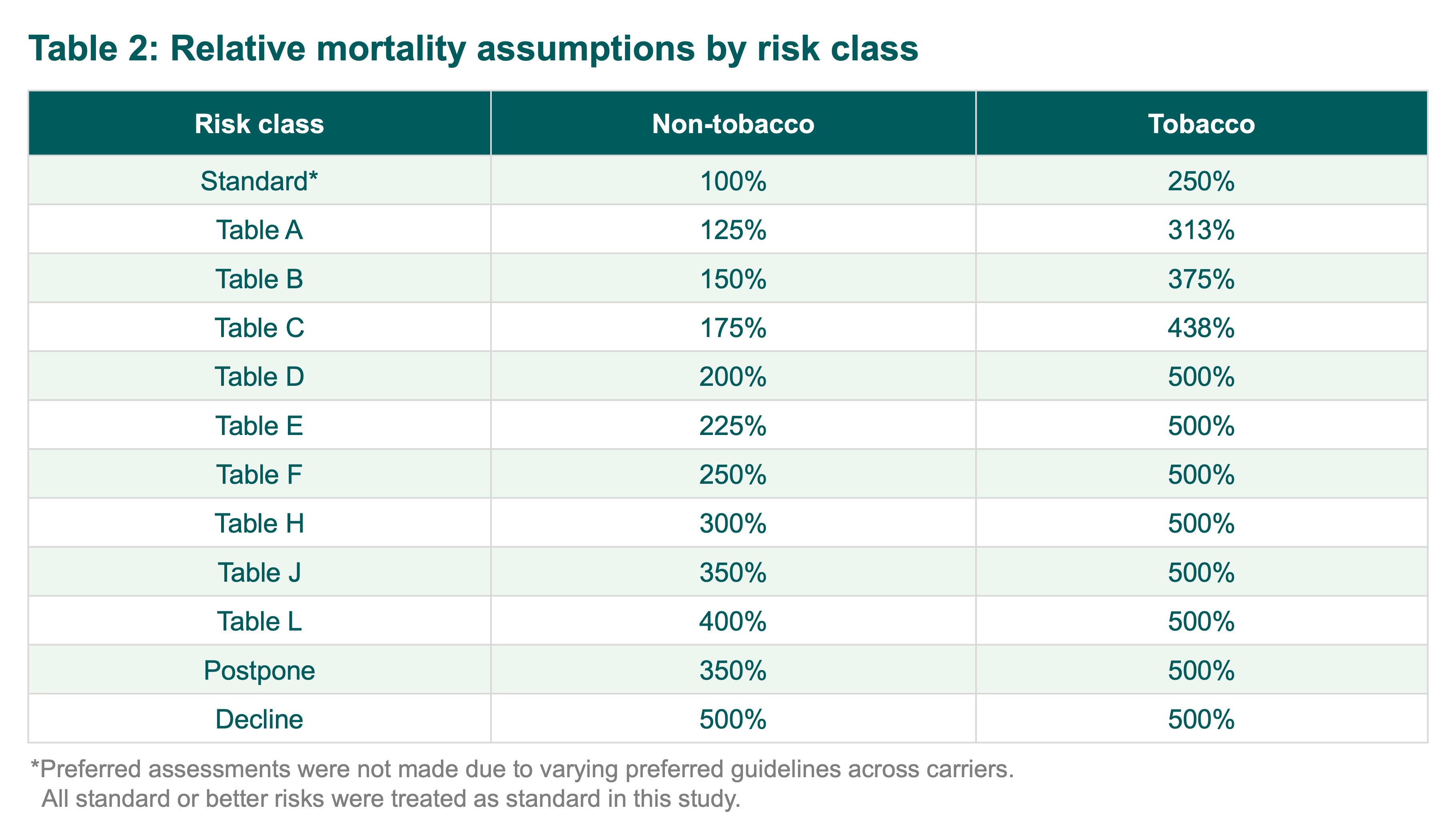
- Table 2 shows the relative mortality assumptions by risk class that were used in the analysis.
- A count-based average expected mortality was calculated based on the relative mortality factors outlined above. There were policies for which an assessment could not be made based on the available underwriting evidence. These undetermined underwriting risks were excluded from the mortality calculation, and therefore, the average expected mortality includes all policies that received an assessment within each simulated underwriting program
- Mortality saving was calculated as follows:
Mortality saving % = (Average expected mortality for Leading with EHRs / Average expected mortality for Traditional AUW) - 1
Results
Decision rates
The Leading with EHRs scenario shows significant operational value by driving a net increase in the number of final decisions that can be made without additional evidence, such as insurance labs or attending physician statements, within an AUW or light touch model.
In an accelerated underwriting context, Leading with EHRs could significantly reduce knockouts and refer-to-underwriter actions, improving instant decision and light touch rates.
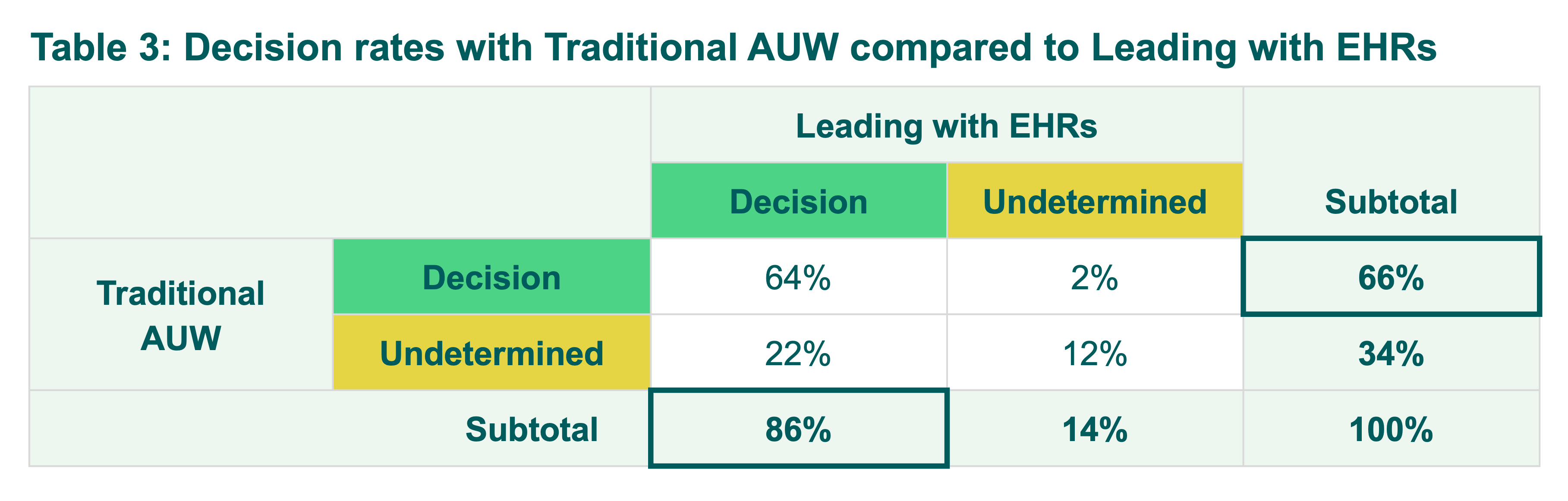
Table 3 compares underwriting outcomes for the same set of applications under both approaches and should be read left to right, with each row showing how Traditional AUW outcomes shift when EHRs are introduced first. It illustrates how the introduction of EHRs shifts cases from “undetermined” to final decisions, as well as the small number of cases that move in the opposite direction.
As shown in Table 3, 66% of cases received a decision under the Traditional AUW approach. When EHRs were introduced as the first piece of evidence, outcomes shifted in two ways:
- Additional cases that were previously undetermined received a decision (22% of total cases), and
- A small number of cases were newly identified as undetermined due to conditions uncovered in the EHR (2% of total cases).
The net impact is an increase in the decision rate from 66% to 86%. Decision rates include decline and postpone assessments; therefore, the percentages of policies receiving actual offers are lower.
Note that Table 3 shows the cumulative decision rate from Leading with EHRs, including decisions both from cases that were decided without medical billing data and cases where medical billing data was ordered reflexively when the EHR either lacked prescription data or other information needed to render an underwriting decision.
In this study, 69% of EHRs contained prescription data, and 75% of those records contained the information needed to support an underwriting decision. As a result, 52% of total study cases could be decisioned based on an EHR alone, without ordering additional medical billing code data.
Mortality savings
The decision changes resulting from the Leading with EHRs scenario yield 25% higher mortality compared to decisions based on the Traditional AUW scenario. Essentially, the medical information uncovered in EHRs enables a more accurate, but potentially more adverse, risk class assessment compared with Traditional AUW, which offsets potential mortality slippage of 25%.
The mortality-saving benefit is quantified at $752 for an average policy.3
To further illustrate the protective value of Leading with EHRs, we examined 92 cases where both the Leading with EHRs scenario and the Traditional AUW scenario produced a decision, and we can directly compare how well each approach protected against mortality slippage.
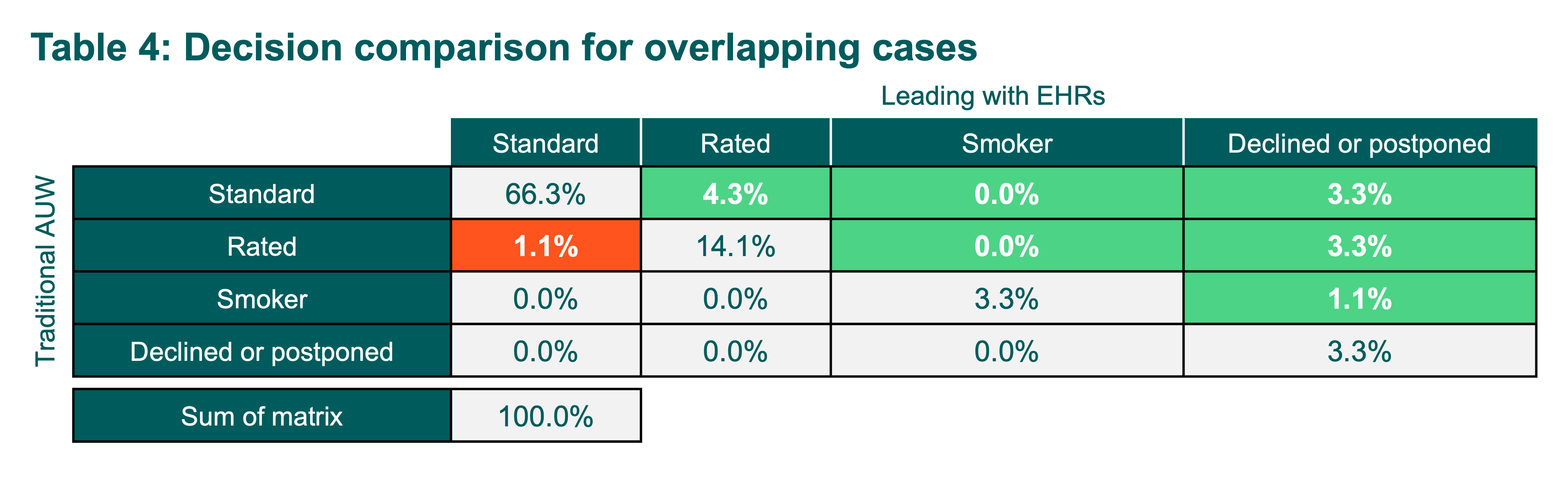
Table 4 compares underwriting outcomes for the same set of applications under both approaches and should be read left to right, with each row showing how Traditional AUW decisions shift when EHRs are introduced first. It highlights where EHRs result in more protective mortality classifications, as well as the small number of cases that move in the opposite direction. Overall, Leading with EHRs correctly identified cases that Traditional AUW would have underassessed. The green cells represent cases where Leading with EHRs provided stronger mortality protection than Traditional AUW. Across the 92 overlapping decisions:
- In 12% of cases (green boxes), Leading with EHRs resulted in a more protective decision, either by identifying impairments missed by Traditional AUW or by assigning a more appropriate risk class.
- In only 1% of cases (red box), Leading with EHRs resulted in decisions that were less protective than Traditional AUW.
For this study, the average cost of EHRs per policy, accounting for 1.4x EHR data sources per life and summarization services, is assessed to be $50 per policy.4 After factoring in the EHR costs, this analysis demonstrates clear net positive protective value, with an average net saving of $702 per policy. (Savings associated with reduced use of billing data are not included in this assessment.)
While the study demonstrates positive net savings at the aggregate level, we further analyzed how net savings vary across issue age and face amount groups. Table 5 illustrates the average net savings per policy at varying issue age and face amount categories.5
Mortality saving calculated by applying the mortality saving percent as a multiplicative factor applied to the Present Value of Death Benefits (PVDB).

Case counts are limited in the above split by age and amount, but findings are largely in line with previous studies, which observed that net savings are, in general, higher at older issue ages and higher face amount bands.
It is also worth noting that leading with EHRs results in positive net mortality savings across all age and amount bands investigated.
Cost-benefit analysis
The mortality savings from Leading with EHRs are significant, but the overall value extends beyond protection to include evidence and underwriting expense reductions. These savings are driven by a reduced proportion of applications requiring full underwriting and lower medical billing code data costs.
Expense savings can vary significantly by program, but based on a typical AUW program, Leading with EHRs can generate approximately $29 in evidence and underwriter time savings per application compared to Traditional AUW.6 Note these expense savings are net of the cost of the EHR evidence, as well as any additional cost of underwriting review from adding an EHR to an underwriting workflow.
When combined with the mortality savings observed in this analysis, Leading with EHRs has the potential to deliver up to $781 in total savings per application, though actual results will vary by case.
These savings are significant, though slightly lower than the $916 average net savings in our previous study assessing adding EHRs as an additional piece of evidence in the accelerated underwriting process. While differences in case counts limit direct comparisons, the results highlight the ability of EHRs to add value across programs with varying evidence expense appetites and underscore the importance of customizing retrospective studies to specific programs.
Considerations for the Leading with EHR use case in the context of EHR development
Utilizing medical data within the underwriting process is not without challenges. Inconsistent levels of data content and variable release rates continue to impact the speed of innovation across states when integrating EHRs into automated underwriting workflows.
Internal performance metrics from MIB EHR, a Munich Re strategic partner, illustrate both the progress and current limitations of EHR retrieval capabilities. For example, approximately 80% of records within MIB’s network are returned within 24 hours, with about 20% returned in under five minutes. Retrieval performance also varies geographically: MIB EHR reports a nationwide release rate of 53% as of the 1st quarter of 2026 with more than 23 states return records in over 50% of searches within MIB’s network, while other states show lower return success.7
MIB EHR has recently expanded access across 16 additional states, including large-volume markets such as California, New Jersey, and Texas. Further expansion is anticipated in 2026 through the adoption of Individual Access Services (IAS), a consumer‑mediated data retrieval model expected to broaden the availability of electronic medical records accessible for underwriting purposes. These developments aim to improve coverage, consistency, and utility of electronic medical data for underwriting evaluation.
While retrieval speed and coverage continue to improve, the extent to which returned records are underwriting‑ready can vary. In some cases, returned records may lack the clinical detail needed to resolve specific underwriting questions. When this occurs, underwriters may revert to more traditional, and often slower, methods to complete the assessment.
Even with these considerations in mind, the findings from this study demonstrate that EHR retrieval early in the underwriting process – with reflexive referral to additional evidence as needed – could significantly improve risk assessment outcomes by enhancing mortality protection, automation rates, and streamlining the applicant experience by reducing the frequency of more invasive insurance labs.
Conclusion
This study demonstrates that positioning EHRs as the first piece of underwriting evidence can provide material mortality protective value while improving operational efficiency. By enabling earlier access to clinical data, Leading with EHRs allows underwriters to make more accurate risk assessments and potentially help carriers accelerate more applications without fluid testing.
In addition, it is important to note that implementing EHRs in underwriting may not be a one-size-fits-all proposition. Program design, distribution strategy, and overall risk profile will dictate how and where electronic health data can be most effectively deployed. Understanding how EHRs interact with existing evidence strategies – and how reflexive ordering can be optimized – allows carriers to tailor their approach for maximum efficiency and impact.
As EHR coverage and data content continue to improve, carriers that thoughtfully integrate EHRs at the front of the underwriting process will be positioned to capture gains in decision speed, evidence cost savings, and mortality savings. Munich Re’s strategic partnership with MIB reflects an ongoing commitment to expanding access to electronic medical data and developing advanced data analytics capabilities that support automated and data-driven risk assessment.
References
Related Solutions
Newsletter
properties.trackTitle
properties.trackSubtitle



